Overview
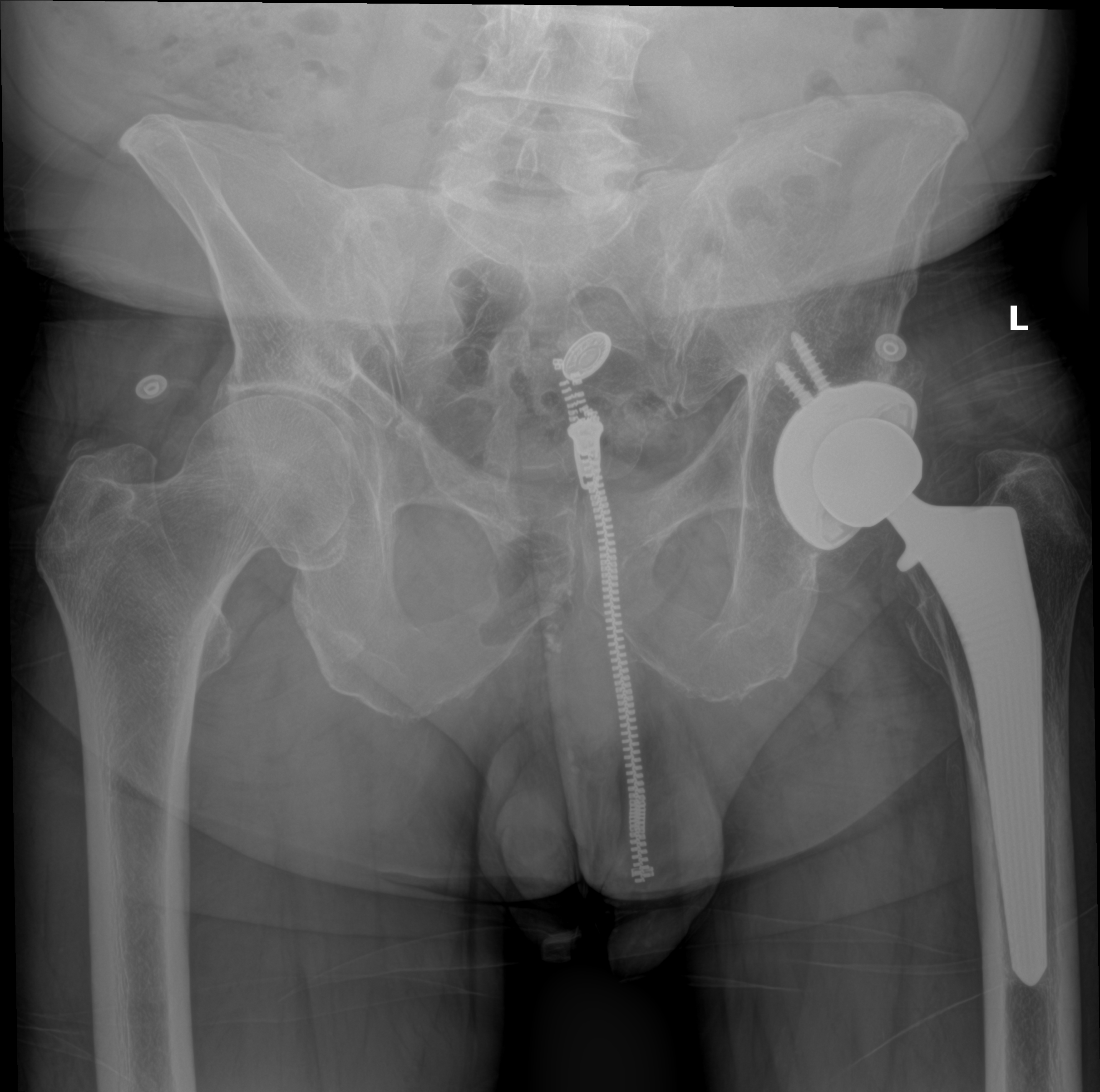
The hip is a ball-and-socket joint formed by the femoral head and the acetabulum of the pelvis. When cartilage wears away — from osteoarthritis, avascular necrosis, inflammatory arthritis, or post-traumatic damage — the bones grind against one another and every step becomes painful. Total hip replacement resurfaces both sides of the joint with a smooth metal-and-polyethylene implant.
How the Procedure Works
We split the gluteus maximus along its fibers and release the short external rotators — piriformis, obturator internus, gemelli — off the posterior femur to access the joint. These are repaired back to bone at closure, which reduces dislocation risk significantly compared to leaving them unrepaired. With the hip dislocated and the femoral head removed, we have excellent visualization of the acetabulum: we ream to the appropriate depth, confirm version and inclination with a trial cup under fluoroscopy, then impact the final metal shell and lock the polyethylene liner. On the femoral side, canal preparation and stem seating are checked for fill and alignment before the final head is placed. Leg lengths are assessed clinically and confirmed on fluoroscopy — a limb length discrepancy of more than a centimeter is one of the most common sources of patient dissatisfaction after hip replacement, and it is largely preventable with careful intraoperative measurement.
When to Consider Posterior Total Hip Replacement
Posterior total hip replacement is generally offered when symptoms, imaging, and a trial of non-operative care together point to surgery as the next step. The typical picture includes:
Pain that limits daily life
Hip pain that interferes with walking, stairs, or sleep despite a full course of anti-inflammatories, therapy, and activity modification.
Radiographic arthritis
X-rays showing joint-space loss, osteophytes, avascular necrosis, or post-traumatic degeneration correlating with symptoms.
Exhausted non-operative care
Failed response to conservative treatment — including weight loss, low-impact exercise, NSAIDs, and intra-articular injections.
Good surgical candidate
Medical optimization completed and no active infection; bone quality and anatomy suitable for implant fixation.
Conditions This Treats
Physicians Who Perform Posterior Total Hip Replacement
Providers Who Surgically Assist with Posterior Total Hip Replacement
Risks & Why We Still Recommend It
Every operation carries risk. The reason we offer this procedure is that the condition, left untreated, causes groin and thigh pain with every step, loss of motion, and progressive loss of the ability to stand, walk, and sleep comfortably. That is the trade we are managing — not eliminating risk, but choosing the smaller of two unfavorable trajectories.
The risks we discuss with patients before posterior total hip replacement include:
- bleeding and infection (including rare deep periprosthetic infection)
- anesthesia risk
- blood clot (DVT/PE) — mitigated by perioperative prophylaxis
- dislocation, particularly in the early recovery phase
- leg-length discrepancy
- sciatic nerve injury (rare)
- periprosthetic fracture
- component loosening or wear over time
If you have had a prior hip replacement
If you have a hip replacement — from here or from elsewhere — and are experiencing new pain, instability, or giving way that is not settling, call our office before booking a clinic visit. Dr. Vrana performs selective revision hip arthroplasty here when the case fits the practice; complex acetabular reconstruction and some multi-component revisions are better handled at a revision-specialty center, and our team can usually tell on the phone which yours is. Learn more about revision total hip replacement →
The indication to proceed is end-stage hip arthritis with daily pain and functional loss that has not responded to non-operative care. Patients who don't need this operation don't get it.
Further Reading
External patient-education references and related OSI pages for additional background:





