Overview
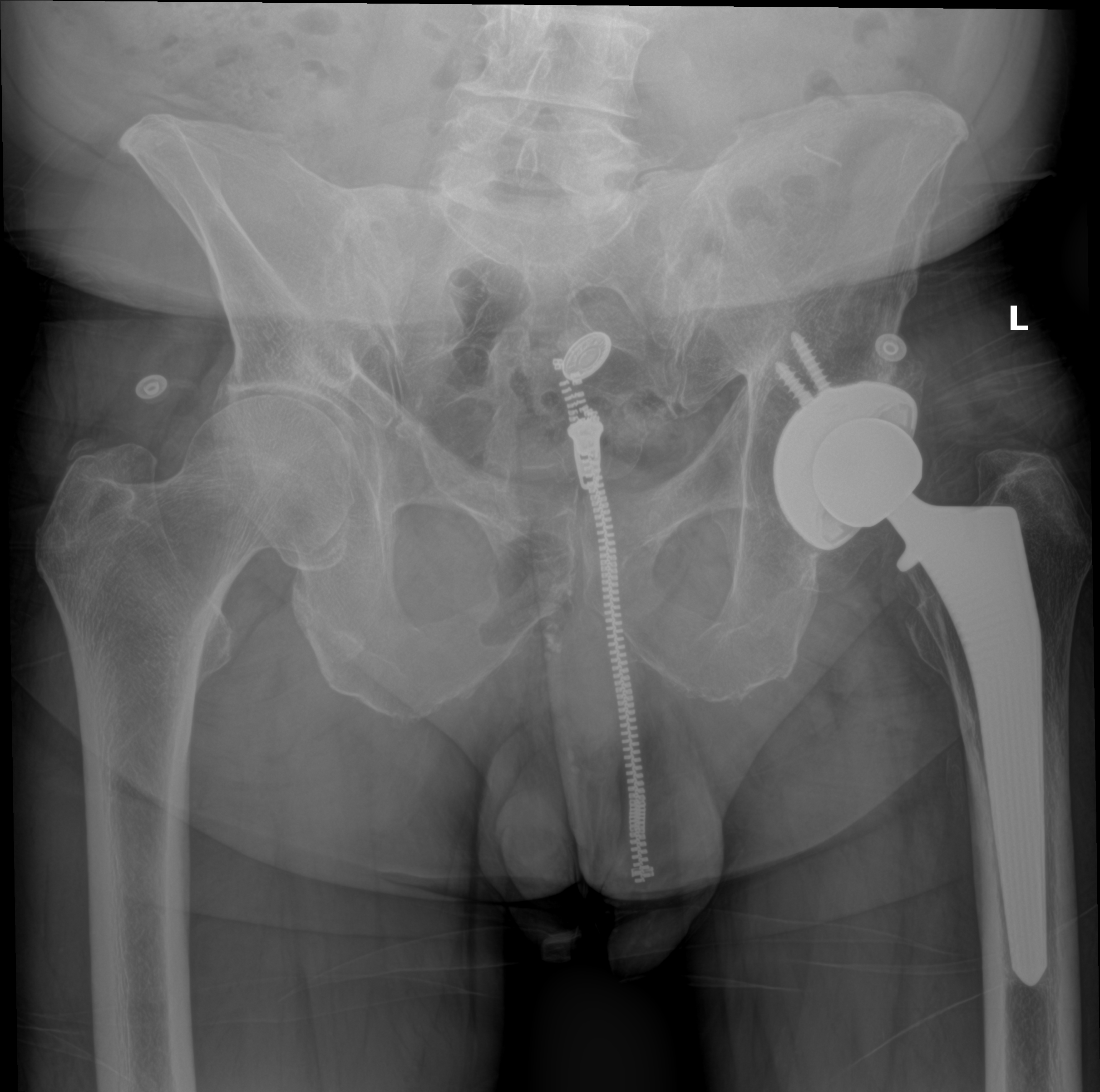
The hip is a ball-and-socket joint formed by the femoral head and the acetabulum of the pelvis. When cartilage wears away — from osteoarthritis, avascular necrosis, inflammatory arthritis, or post-traumatic damage — the bones grind against one another and every step becomes painful. Total hip replacement resurfaces both sides of the joint with a smooth metal-and-polyethylene implant.
The direct anterior approach replaces the same arthritic hip as a posterior replacement, but enters the joint through a natural plane between muscles rather than cutting through them. Because no muscle is detached from bone, the posterior capsule and gluteal muscles stay intact — which translates into fewer motion restrictions and often a faster early recovery. The final hardware and alignment are the same whether the joint is reached anteriorly or posteriorly; only the path of dissection differs.
How the Procedure Works
The anterior approach replaces the same arthritic joint as a posterior hip, but the distinction is that no muscle is cut or detached from bone. The steps below describe how we enter through a natural plane and keep it that way.
Intermuscular interval and joint exposure
We work through the Hueter interval — the plane between the tensor fasciae latae laterally and the sartorius medially. No muscle is cut and no tendon is released; the plane is developed, not created. The anterior capsule is opened and the femoral head delivered, with the patient positioned on a traction table so the operative leg can be controlled in extension, abduction, and rotation.
Femoral neck osteotomy and head removal
The femoral neck is cut at a pre-planned level based on preoperative templating, and the arthritic head is removed. The cut level sets leg length and offset for the rest of the case, so it is measured, not estimated. Any anterior osteophytes impinging on the psoas are cleared at the same time.
Acetabular reaming and cup placement
The acetabulum is reamed progressively until healthy subchondral bone supports the full hemisphere. A press-fit cup is impacted with deliberate version and inclination; a few degrees in either direction meaningfully changes dislocation risk and polyethylene wear. Fluoroscopy is used intraoperatively to confirm cup position against a true pelvic reference, rather than relying on visual estimation through a small anterior window.
Femoral preparation
Exposing the femur anteriorly is the demanding part of the operation. The leg is hyperextended, externally rotated, and adducted to deliver the proximal femur into the wound; the posterior capsule is selectively released only as needed for exposure, never routinely. The canal is broached sequentially until the stem fits the metaphysis with rotational stability.
Trial reduction, leg length check, and final seating
A trial head is placed and the hip reduced, then leg lengths and offset are confirmed on fluoroscopy and against the contralateral side. Stability is tested through range of motion before components are finalized. The final stem is impacted, a ceramic or metal head is seated, and the anterior capsule is repaired — leaving the posterior capsule and gluteal muscles untouched, which is why traditional posterior hip precautions are not needed afterward.
When to Consider Anterior Total Hip Replacement
Anterior total hip replacement is generally offered when symptoms, imaging, and a trial of non-operative care together point to surgery as the next step. The typical picture includes:
Arthritis that limits function
Hip pain from osteoarthritis, avascular necrosis, or dysplasia that hasn't responded to non-operative care.
Preference for fewer restrictions
Patients who want to skip the strict posterior hip precautions and get back on their feet sooner.
Anatomy suited to the approach
Body habitus and femoral anatomy that allow safe anterior exposure — evaluated preoperatively with imaging.
Conditions This Treats
Physicians Who Perform Anterior Total Hip Replacement
Providers Who Surgically Assist with Anterior Total Hip Replacement
Risks & Why We Still Recommend It
Every operation carries risk. The reason we offer this procedure is that the condition, left untreated, causes groin and thigh pain with every step, loss of range of motion, and a progressive shortening of the affected limb. That is the trade we are managing — not eliminating risk, but choosing the smaller of two unfavorable trajectories.
The risks we discuss with patients before anterior total hip replacement include:
- bleeding and infection (including rare deep periprosthetic infection)
- anesthesia risk
- blood clot (DVT/PE) — mitigated by perioperative prophylaxis
- dislocation (less common with the anterior approach but still possible)
- leg-length discrepancy
- lateral femoral cutaneous nerve irritation causing anterior thigh numbness, usually transient
- periprosthetic fracture, particularly on the femoral side
- component loosening or wear over time
If you have had a prior hip replacement
If you have a hip replacement — from here or from elsewhere — and are experiencing new pain, instability, or giving way that is not settling, call our office before booking a clinic visit. Dr. Vrana performs selective revision hip arthroplasty here when the case fits the practice; complex acetabular reconstruction and some multi-component revisions are better handled at a revision-specialty center, and our team can usually tell on the phone which yours is. Learn more about revision total hip replacement →
The indication to proceed is end-stage hip arthritis with daily pain and functional loss that has not responded to non-operative care. Patients who don't need this operation don't get it.
Further Reading
External patient-education references and related OSI pages for additional background:





