Overview
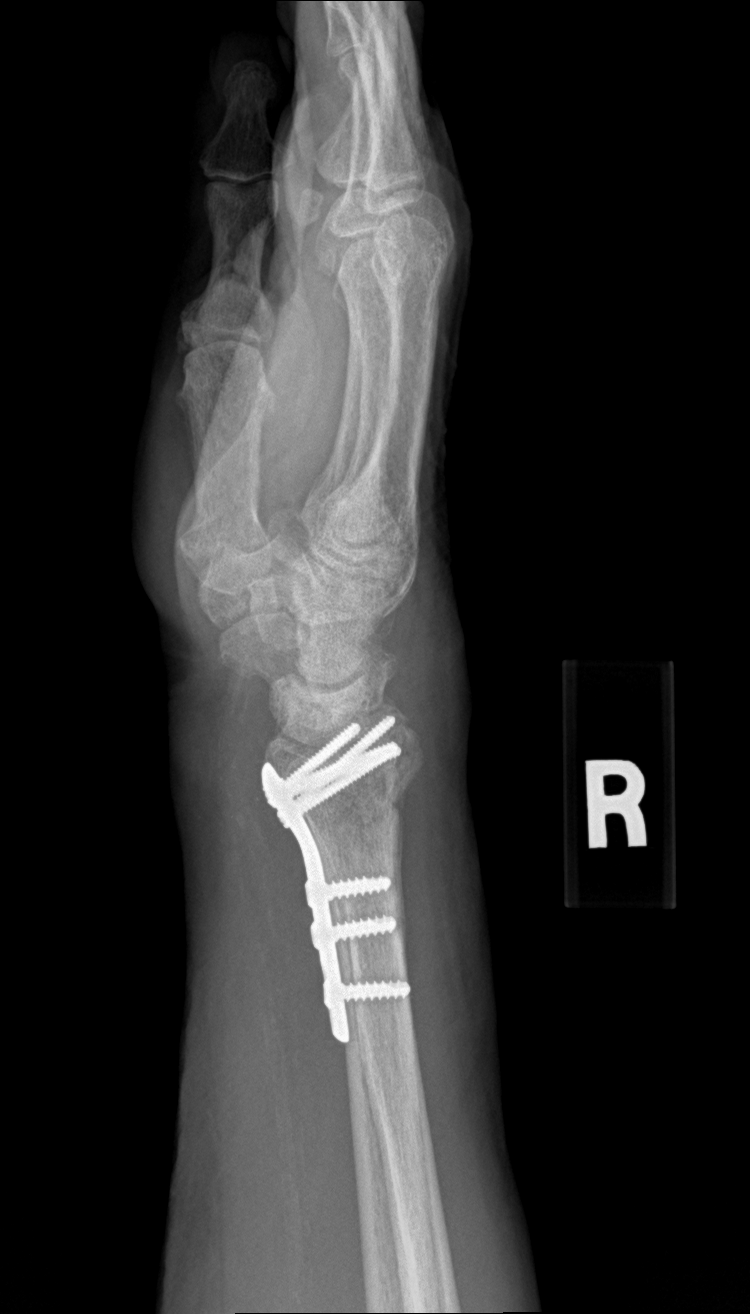
The distal radius is the most commonly fractured bone in the adult skeleton. When the fracture is displaced, unstable, or extends into the wrist joint surface, casting alone will not hold alignment. Surgical fixation restores length, angulation, and joint congruity — important for long-term wrist function and cosmetic appearance.
How the Procedure Works
We approach through a volar (palm-side) incision, working through the interval between the flexor carpi radialis and the radial artery — this gives direct access to the fracture while keeping extensor tendons and the dorsal sensory branch of the radial nerve out of harm's way. The fracture is reduced under fluoroscopy: we restore radial length, volar tilt, and radial inclination to within a few degrees of the uninjured side, because small residual malreduction of the joint surface accelerates wrist arthritis. A pre-contoured locking plate sits against the volar cortex; subchondral screws through the distal row lock the articular fragments in position from below, supporting the joint surface the way scaffolding supports a ceiling. Fluoroscopy in multiple planes confirms screw length — dorsal screw penetration into the extensor tendons is a known complication, avoided by careful intraoperative imaging. Rigid fixation means the patient starts wrist motion early rather than spending an extended period in a cast.
When to Consider Distal Radius ORIF
Distal radius ORIF is generally offered when symptoms, imaging, and a trial of non-operative care together point to surgery as the next step. The typical picture includes:
Displaced or unstable fracture
A fracture that has shortened, angulated, or displaced beyond acceptable limits — or one likely to do so in a cast.
Intra-articular step-off
A fracture that crosses into the wrist joint surface with a step that must be reduced to preserve long-term function.
Active patients
Patients requiring an early return of wrist function for work or activity.
Conditions This Treats
Physicians Who Perform Distal Radius ORIF
Providers Who Surgically Assist with Distal Radius ORIF
Weight-Bearing After Repair
Controlled load is part of how bone heals. Once the fracture is stabilized with hardware, gentle weight through the limb stimulates the biology that builds callus and remodels bone — completely offloading a fixed fracture for too long can actually slow healing and stiffen the joint above and below. Full body weight right away, however, can overload the construct before bone has caught up. The right answer sits in between: a partial weight-bearing progression decided by your surgeon based on your fracture pattern, the strength of the fixation, your bone quality, and how the repair looks on post-op imaging. We tell you exactly how much weight the limb can take, when to advance, and what to watch for.
Risks & Why We Still Recommend It
Every operation carries risk. The reason we offer this procedure is that the condition, left untreated, causes a wrist fracture that heals malaligned, producing weak grip, limited motion, and early wrist arthritis. That is the trade we are managing — not eliminating risk, but choosing the smaller of two unfavorable trajectories.
The risks we discuss with patients before distal radius orif include:
- bleeding and infection
- anesthesia risk
- stiffness
- tendon irritation or rupture from hardware prominence (particularly extensor pollicis longus and flexor pollicis longus)
- median nerve irritation or carpal tunnel syndrome
- CRPS (uncommon but specific to the distal radius)
- loss of reduction
The indication to proceed is a displaced distal radius fracture that cannot be held reliably in a cast. Patients who don't need this operation don't get it.
Further Reading
External patient-education references and related OSI pages for additional background:





